Vitrectomy is a microsurgical procedure in which the vitreous humor, the gel filling the eye, is removed to allow the surgeon to treat diseases of the retina and vitreous. Removing this gel permits removal of blood, scar tissue or foreign objects, repair of detachments and macular holes, treatment of infections and delivery of medications. After the gel is removed, the eye is filled with a clear substitute, such as saline, a gas bubble or silicone oil, to support the retina during healing.
Vitrectomy
Types of Vitrectomy
Posterior (pars plana) vitrectomy is performed through tiny incisions in the pars plana, a region of the eye’s white wall located behind the iris. Modern systems use small-gauge instruments (23-, 25- or 27-gauge) that are self-sealing, resulting in minimal discomfort and faster recovery. Anterior vitrectomy is done when the vitreous prolapses into the front chamber, such as after cataract surgery complications or trauma, to prevent lens or corneal damage. Nearly all retina specialists perform pars plana vitrectomy, while many ophthalmologists perform anterior vitrectomy when needed.
Preoperative Evaluation
Before surgery, the patient undergoes a full eye examination and imaging (such as OCT or ultrasound) to assess the condition. Systemic diseases like diabetes, hypertension or heart disease must be controlled. The surgeon discusses the risks, benefits and alternatives, ensuring that the patient understands the need for surgery. Preoperative instructions may include fasting, adjusting medications and arranging transportation since vision will be impaired after surgery.
Procedure Details
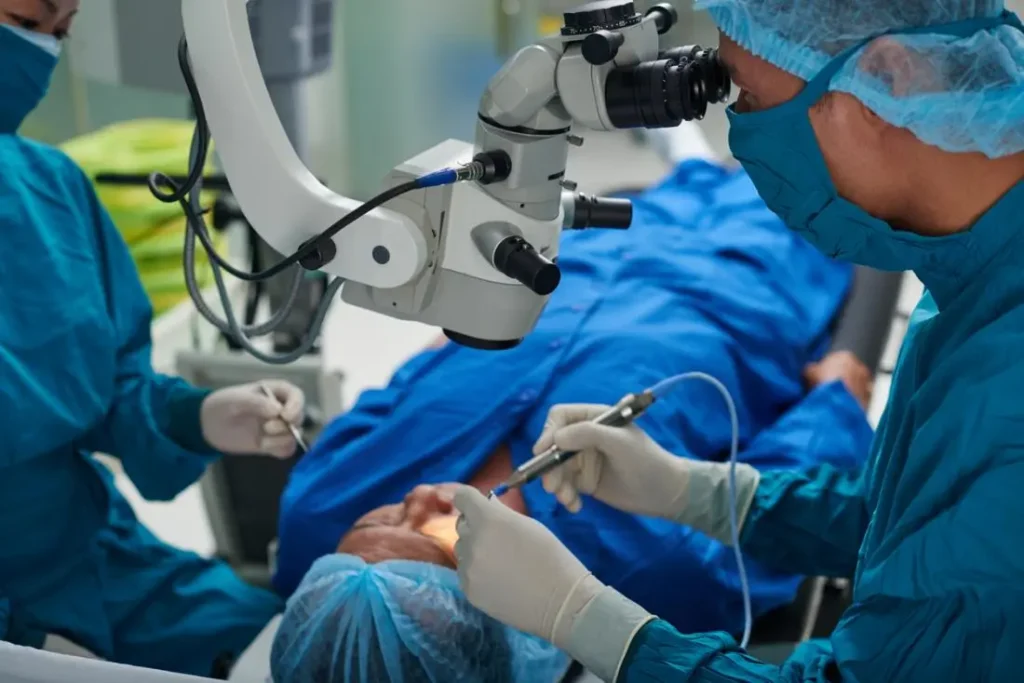
Most vitrectomies are outpatient procedures performed under local anesthesia with intravenous sedation. The operative eye is numbed with injections or topical anesthetic. After sterile preparation and placement of an eyelid speculum to keep the eye open, three tiny incisions are made in the pars plana. Through these openings, the surgeon inserts a light pipe to illuminate the eye, a vitrectomy probe to cut and remove the gel, and various instruments such as forceps for membrane peeling and drainage needles for fluid removal. A wide-angle viewing system provides magnified views of the retina. Once the gel and any pathological tissue are removed, the surgeon may inject saline, a gas bubble or silicone oil to fill the eye. Gas bubbles slowly resorb over days to weeks, while silicone oil may require a later removal.
Postoperative Care and Recovery
After surgery, the eye is patched and patients are monitored before going home. Antibiotic and anti-inflammatory drops are prescribed. If a gas bubble is used, patients must maintain specific head positions, often face-down, to keep the bubble against the retina. They should avoid air travel until the bubble dissipates because pressure changes can damage the eye. Vision is usually blurry immediately after surgery and improves gradually as the bubble absorbs and the retina heals. Full recovery may take several weeks to months. The typical follow-up schedule includes day one, one week, one month appointments during which it is important to monitor eye pressure.
Vitrectomy Goals
Risks and Complications
Vitrectomy is generally safe and success rates exceed 90 percent for many indications. Potential complications include infection, bleeding, increased or decreased eye pressure, cataract formation, new retinal tears or detachment and persistent inflammation. The likelihood of cataract progression is high in patients over fifty undergoing vitrectomy; combined cataract and vitrectomy surgery is common. Patients should understand that additional surgery may be needed, for example to remove silicone oil or to address recurrent membrane formation.
Alternatives and Adjuncts
There are also non-surgical or less invasive alternatives. Vision-blocking floaters might be treated with laser vitreolysis. Some macular holes may close spontaneously or respond to face-down positioning without surgery. For diabetic retinopathy, intravitreal injections and laser photocoagulation may stabilize disease without vitrectomy. However, once traction or hemorrhage threatens vision, vitrectomy often offers the best chance for improvement. Adjunct procedures such as scleral buckle or laser photocoagulation are often performed together with vitrectomy to address underlying pathology.
Outcomes
Outcomes depend on the underlying condition, duration of vision loss and patient factors. In cases like vitreous hemorrhage from diabetic retinopathy, vision often improves dramatically after surgery. For macular holes or epiretinal membranes, many patients regain reading vision, though some distortion may persist. When vitrectomy repairs a retinal detachment, visual recovery depends on macular involvement. Depending on severity it is important to have timely surgery, adhere to postoperative instructions and attend regular follow-up care. Patients should discuss individual prognosis with their surgeon.
Our Practice Locations and Physicians
With six locations across the upstate, our team is able to conveniently serve you in treating your macular degeneration.
Learn more about our locations and the physicians serving at each practice.
