Click on any term below to open up the definition, along with additional resources for learning more
Resources
Further Study and Understanding
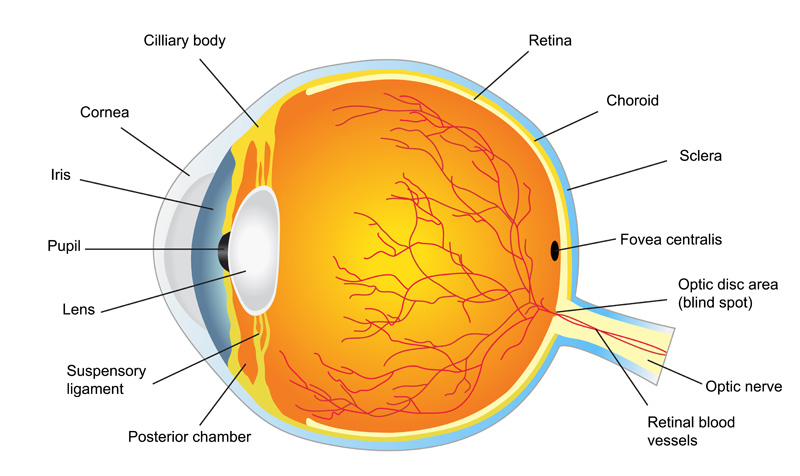
Eye Terminology
The retina is the light-sensitive tissue in the back of the eye. The sensory membrane that lines most of the large posterior chamber of the eye. The Retina is composed of several layers including one containing the rods and cones, and functions as the immediate instrument of vision by receiving the image formed by the lens and converting it into chemical and nervous signals which reach the brain by way of the optic nerve.
The macula is the part of the retina that is responsible for your central vision, allowing you to see fine details clearly.
The optic nerve is the largest sensory nerve of the eye. It transmits impulses to the brain from the retina.
The choroid is the pigmented vascular layer of the eyeball between the retina and the sclera.
The retina contains two types of photoreceptors: rods and cones. Rods contain only one type of light sensitive pigment and are responsible for peripheral and night vision. Cones are responsible for your ability to see during the day, in color and in detail.
Common Problems Descriptions and Terminology
Age-related macular degeneration (AMD) is a deterioration or breakdown of the eye’s macula. The macula is a small area in the retina—the light-sensitive tissue lining the back of the eye. The macula is the part of the retina that is responsible for your central vision, allowing you to see fine details clearly. Dry AMD is most common type of macular degeneration and affects 90% of the people who have the condition. In the dry form, there is a breakdown or thinning of the layer of retinal pigment epithelial cells (RPE) in the macula. Wet AMD occurs when abnormal blood vessels behind the retina start to grow under the macula. These blood vessels often leak blood and fluid, damaging or killing light-sensitive cells—loss of vision occurs quickly.
Links:
In central serous retinopathy (sometimes called central serous choroidopathy), fluid builds up under the retina and distorts vision. A small detachment forms under the retina as a result, causing the vision to be distorted.
CMV is a common virus caused by a group of herpes-type viruses that can affect almost anyone. It is spread through body fluids and most commonly affects people with weakened immune systems. Symptoms may include blind spots, blurred vision and/or floaters.
Diabetic retinopathy, the most common diabetic eye disease, occurs when blood vessels in the retina change. Sometimes these vessels swell and leak fluid or even close off completely. Fluid can leak into the center of the macula and cause macular edema. In other cases, abnormal new blood vessels grow on the surface of the retina. All people with diabetes are at risk of developing diabetic retinopathy and it is important to receive a comprehensive dilated eye exam at least once a year.
Links:
You may sometimes see small specks or clouds moving in your field of vision. These are called floaters. When the vitreous gel pulls on the retina, you may see what look like flashing lights or lightning streaks. These are called flashes. It is common to experience these symptoms as the vitreous gel pulls away from the retina as we age.
A macular hole is a small break in the macula, the part of your eye responsible for detailed, central vision. As we age, the vitreous shrinks and pulls away from the retina. If the vitreous is firmly attached to the retina as it pulls away, it can cause the retina to tear and create a macular hole. A macular hole can cause blurred and distorted central vision and are usually related to aging and occurs in people over age 60.
Links:
A macular pucker (also called an epiretinal membrane) is a layer of scar tissue that grows on the surface of the retina, particularly the macula, which is the part of your eye responsible for detailed, central vision. As we age, the vitreous gel begins to pull away from the macula and sometimes scar tissue may develop as a result. Scar tissue can cause the retina to become swollen or distorted and vision can become blurry.
Links:
Toxoplasmosis is an infection caused by the parasite, Toxoplasma gondii. The toxoplasma organism resides in the intestinal tracts of many animals, particularly cats. The infectious organisms are transmitted by ingestion. Newly infected persons may not experience any symptoms but symptoms may occur one to two weeks after exposure. The infection can cause significant inflammation and scarring which may impair vision.
Histoplasmosis is a disease caused by the fungus histoplasma capsulatum. This fungus is found all over the world and derives from river valleys and soil where bird or bat droppings may be found. The fungus may be released into the air and inhaled into the lungs causing the infection. OHS may develop when abnormal blood vessels grow under the retina. Those blood vessels form a lesion and, if left untreated, can cause the normal tissue to be replaced by scar tissue. Vision may become impaired, and that is why early treatment is important.
Usually, the vitreous moves away from the retina without causing problems. But sometimes the vitreous pulls hard enough to tear the retina in one or more places. Fluid may pass through a retinal tear, lifting the retina off the back of the eye — much as wallpaper can peel off a wall. When the retina is pulled away from the back of the eye like this, it is called a retinal detachment.
Links:
The retina—the layer of light-sensitive cells at the back of the eye—is nourished by the flow of blood, which provides nutrients and oxygen that nerve cells need. When there is a blockage in the veins into the retina, retinal vein occlusion may occur.
Links:
Retinitis pigmentosa is an inherited retinal disorder that primarily affects the rods—the photoreceptors (light-sensing cells) responsible for peripheral (side) and night vision. The name retinitis pigmentosa refers to the characteristic finding of pigmentary (color) changes seen with a dilated eye examination.
Links:
Retinoschisis occurs when there is a separation between the two major layers of the retina. This can be caused by aging when cysts form within the retina. If the cysts combine, the retina will form a retinoschisis. Retinoschisis, typically, does not cause any symptoms. The layers may develop retinal holes, which could progress to a retinal detachment if fluid leaks below the two layers.
A Vitreous hemorrhage occurs when blood leaks into the areas in and around the vitreous humor of the eye.
Diagnostic Testing Descriptions and Terminology
Fluorescein angiography is an eye test that uses a special dye and camera to look at blood flow in the retina and choroid, the two layers in the back of the eye. A dye called fluorescein is injected into a vein and a special camera is used to capture images of the inside of the eye as the dye moves through the blood vessels.
Optical coherence tomography (OCT) is a non-invasive imaging test that uses light waves to take cross-section pictures of your retina, the light-sensitive tissue lining the back of the eye.
A procedure similar to fluorescein angiography, ICG angiography uses Indocyanine Green dye, which fluoresces in the infra-red (non-visible) light. The infra-red wavelengths have the ability to penetrate the retinal layers making the circulation in deeper layers visible when photographed with an infra-red sensitive camera.
Treatments Descriptions and Terminology
Laser surgery shrinks abnormal blood vessels and reduces macular swelling. This type of treatment is recommended for people with macular edema and proliferative diabetic retinopathy (PDR).
Pneumatic Retinopexy is a procedure to repair rhegmatogenous retinal detachments. This type of procedure is a non invasive method for retinal detachment repairs. The doctor injects a gas bubble into the vitreous cavity and laser treatment may also be combined during the procedure. The bubble pushes the tear back into place and the bubble will gradually disappear. Head positioning is a requirement after surgery, to allow the bubble to stay in place.
This type of treatment is performed as an outpatient procedure and is used to repair a retinal detachment. A flexible band is placed around the eye to prevent force from pulling the retina out of place.
The most common conditions requiring vitreous surgery are retinal detachment, macular pucker, retinal tears, intraocular infections, endophthalmitis, traumas, intraocular foreign bodies, and macular holes. Vitreous surgery is performed in an operating room under local or general anesthesia. The vitreous is removed and replaced, with either clear fluid that is compatible with the eye, or with a gas that completely fills the eye. Over time, the fluid (or gas) is absorbed by the eye and is replaced by the eye’s own fluid; the eye does not replace the vitreous gel itself. The lack of vitreous gel does not affect the functioning of the eye. A laser probe can be inserted into the eye so that laser treatment can be done during surgery
Have Questions About A Diagnosis or Treatment Plan?
We are here to help! Please don’t hesitate to reach out.
